TTS 2020 Virtual Congress - Thank You!

JUST RELEASED - TRANSPLANTATION DIRECT - OCTOBER ISSUE
The October issue of Transplantation Direct is ready for viewing. This issue covers various topics, including an interesting basic science report on certain HLA-DR types that may cause self-antigen responses promoting chronic rejection after lung or heart transplantation. Two articles address immunosuppression issues: one focuses on the metabolism of tacrolimus by gut bacteria and the other looks at what to do in a case of supratherapeutic overdosing of MMF. An article in kidney transplantation looks at how distance between dialysis and transplant centers affects transplantation rates. There are several articles in the area of liver transplantation, including guidance on opportunities for physicians to prescribe medication for alcohol use disorder. The association of hyponatremia on waitlist mortality in pediatric liver transplant candidates is investigated. A study on transplant outcomes in NAFLD patients with HCC is reported on. There also a case report on the treatment of a patient with Alagille syndrome that had recurrent HCC. In lung transplantation, the use of plasma donor-derived cell-free DNA as a marker of acute rejection is investigated. We also have a retrospective cohort study on the issue of frailty in simultaneous pancreas-kidney transplantation, looking specifically at sarcopenia as a predictor of outcomes. For further details on these articles, please visit our Transplantation Direct open access website.
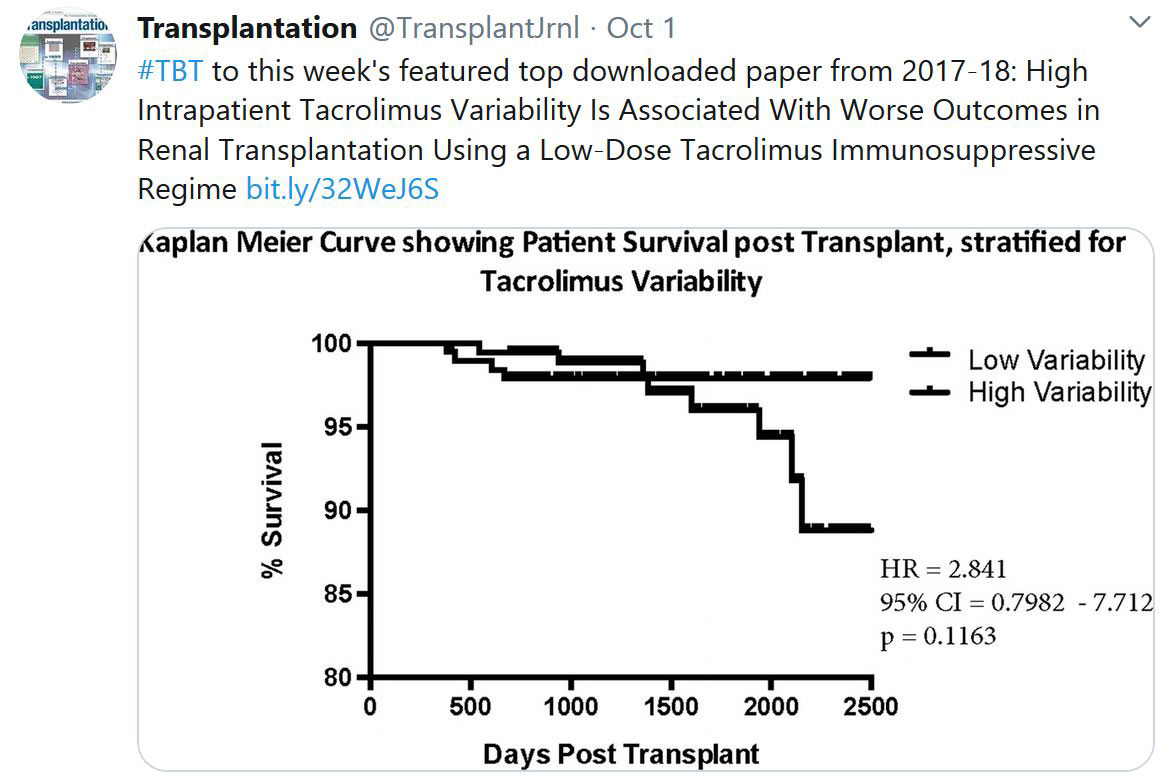
TRANSPLANTATION - WEEK'S MOST DOWNLOADED PAPER
«HOT OFF THE PRESS»
RECENT PUBLICATIONS IDENTIFIED BY TTS EDUCATION COMMITTEE ON COVID-19
Prevalence of SARS-CoV-2 antibodies in a large nationwide sample of patients on dialysis in the USA: a cross-sectional study
Shuchi Anand et al.
Lancet. Published Online September 25, 2020 https://doi.org/10.1016/ S0140-6736(20)32009-2
This article tested the remainder plasma of 28 503 randomly selected adult patients receiving dialysis in July, 2020 in 1300 dialysis facilities across USA, using a spike protein receptor binding domain total antibody chemiluminescence assay (100% sensitivity, 99·8% specificity). Seroprevalence of SARS-CoV-2 was 8·0% (95% CI 7·7–8·4) in the sample, 8·3% (8·0–8·6) when standardized to the US dialysis population, and 9·3% (8·8–9·9) when standardized to the US adult population. When standardized to the US dialysis population, seroprevalence ranged from 3·5% (3·1–3·9) in the west to 27·2% (25·9–28·5) in the northeast. Residents of non-Hispanic Black and Hispanic neighborhoods experienced higher odds of seropositivity (odds ratio 3·9 [95% CI 3·4–4·6] and 2·3 [1·9–2·6], respectively) compared with residents of predominantly nonHispanic white neighborhoods. Residents of neighborhoods in the highest population density quintile experienced increased odds of seropositivity (10·3 [8·7–12·2]) compared with residents of the lowest density quintile.
Imbalance of regulatory and cytotoxic SARS-CoV-2-reactive CD4+ T cells in COVID-19
Benjamin J. Meckiff et al.
Cell. (2020), doi: https://doi.org/10.1016/j.cell.2020.10.001.
This article presented single-cell transcriptomic analysis of >100,000 viral antigen-reactive CD4+ T cells from 40 COVID-19 patients. In hospitalized patients compared to non-hospitalized patients, increased proportions of cytotoxic follicular helper (TFH) cells and cytotoxic T helper cells (CD4-CTLs) responding to SARS-CoV-2, and reduced proportion of SARS-CoV-2-reactive regulatory T cells (TREG) were found. Importantly, in hospitalized COVID-19 patients, a strong cytotoxic TFH response was observed early in the illness which correlated negatively with antibody levels to SARS-CoV-2 spike protein. Polyfunctional T helper (TH)1 and TH17 cell subsets were underrepresented in the repertoire of SARS-CoV-2-reactive CD4+ T cells compared to influenza-reactive CD4+ T cells.
Clinical features of COVID-19 mortality: development and validation of a clinical prediction model
Arjun S Yadaw et al.
Lancet Digital Health. 2020; 2: e516–25 DOI:https://doi.org/10.1016/S2589-7500(20)30217-X
This study applied machine learning techniques to clinical data from a large cohort of patients with COVID-19 treated at the Mount Sinai Health System in New York City, NY, USA, to predict mortality. Using the development dataset (n=3841) and a systematic machine learning framework, we developed a COVID-19 mortality prediction model that showed high accuracy (AUC=0·91) when applied to test datasets of retrospective (n=961) and prospective (n=249) patients. This model was based on three clinical features: patient’s age, minimum oxygen saturation over the course of their medical encounter, and type of patient encounter (inpatient vs outpatient and telehealth visits).
CORONAVIRUS (COVID-19) UPDATES
INVITATION TO PARTICIPATE

Dear Members,
Researchers at McGill University are currently conducting a study entitled LIST-COVID-19 to study the impact of the COVID-19 pandemic on transplantation activity, volumes and immunosuppression practices on a global scale. The study will also help better understand the current and anticipated risks to transplantation during the pandemic and inform clinical practice during the “ramp-up” phase. The Transplantation Society is supporting the project, as well as several National and International Societies.
They are looking for physicians who take care of patients with a solid organ transplant to take a 10-15 minute survey on behalf of their center and program. Please note this is not a patient registry and no specific patient-level data is being collected. Please be assured they will only perform a collective analysis of the survey questions and no personal information identifying the participants will be divulged. The survey responses will be confidential. If you are interested in participating, please contact them at the emails listed below.
Investigators: Shaifali Sandal, MD and Marcelo Cantarovich, MD
Contact: shaifali.sandal@mcgill.ca and marcelo.cantarovich@muhc.mcgill.ca
The Transplantation Society (TTS) and our journal Transplantation have developed online resources to keep you informed on the Coronavirus (COVID-19) outbreak.
- TTS Coronavirus (COVID-19) Dashboard
www.tts.org/covid-19 - Transplantation Global Transplantation COVID Report
www.tts.org/txjcovid19
We are also requesting contributions and news from the transplant community to be sent to covid-19@tts.org for inclusion on our resources page.
In this dashboard, you will find links to TTS and other global and regional resources, as well as interactive maps, publications and webinars. We encourage you to explore this dashboard and share with your colleagues.
Editors and contributors to Transplantation have shared their thoughts on how they are dealing with the current crisis. While we understand that the information of today may be quite different tomorrow in this fast-moving pandemic, this report will open our forum of an international exchange on COVID for the transplant community.
Website - www.tts.org/txjcovid19
Please send your own contributions and news to covid-19@tts.org for inclusion on our resources page.
IN THE NEWS
A DRONE JUST MOVED A HUMAN KIDNEY ACROSS THE NEVADA DESERT TO PROVE IT COULD BE THE FUTURE OF ORGAN TRANSPORT — TAKE A LOOK

Oct. 1 - MissionGo, a transportation logistics company, partnered with the Nevada Donor Network in a test to fly corneas and kidneys across the desert. MissionGo says the drone delivery can be more efficient, and reduce the carbon footprint of the donations.
AGA RELEASES LARGEST REPORT ON SAFETY AND EFFECTIVENESS OF FECAL MICROBIOTA TRANSPLANTATION
Oct. 1 - the American Gastroenterological Association (AGA) released the first results from the NIH-funded AGA Fecal Microbiota Transplantation (FMT) National Registry, the largest real-world study on the safety and effectiveness of FMT. Published in Gastroenterology, the registry reported that FMT led to a cure of Clostridioides difficile (C. difficile) infection in 90% of patients across 20 North American FMT practice sites. Few serious side effects were reported.
PRETRANSPLANT DIALYSIS MODALITY AND LONG-TERM OUTCOMES IN KIDNEY TRANSPLANTATION
Oct. 1 - For patients with end-stage kidney disease (ESKD), kidney transplantation is the optimal therapy. However, preemptive kidney transplantation is not always possible; patients with ESKD are treated with hemodialysis or peritoneal dialysis while on the transplant waiting list. Data from previous studies of the impact of predialysis modality on patient and graft survival following transplantation were conflicting and the studies lacked sufficient follow-up.
ARE ORGAN TRANSPLANT RECIPIENTS AT GREATER RISK OF DEATH FROM COVID-19?
Oct. 1 - A new study, published in Transplantation, finds that risk of death from COVID-19 in organ transplant recipients may be based upon how the patient was treated. "Using data from the COVID-19 Rapid Response Registry, we examined COVID-19 positive adult solid organ transplant recipients and non-transplant patients that were matched to them on age, race and whether they were admitted at the hospital or seen at an outpatient facility," says lead author of the study, Pratima Sharma, M.D., an associate professor of medicine and a transplant hepatologist at Michigan Medicine.
UPCOMING MEETINGS AND ANNOUNCEMENTS
3rd IPITA/JDRF/HSCI Virtual Summit on Stem Cell Derived Beta Cells
The International Pancreas & Islet Transplant Association (IPITA) Conference Organizing Committee is committed to bringing the community together virtually.
International Transplantation Science Meeting (ITS 2021)

IPITA-IXA-CTRMS Joint Congress
FOCIS 2020 Virtual Annual Meeting
TTS members are invited to attend the FOCIS 2020 Virtual Annual Meeting – THE meeting in translational immunology!
The Federation of Clinical Immunology Societies exists to improve human health through immunology.
The FOCIS 2020 Virtual Annual Meeting on October 28-31, 2020, brings together an interdisciplinary group of world-renowned physicians and researchers to share the latest findings on diseases impacting the immune system.
Asian Transplantation Week (ATW) 2020
Contact
Address
The Transplantation Society
International Headquarters
740 Notre-Dame Ouest
Suite 1245
Montréal, QC, H3C 3X6
Canada
Используйте Вавада казино для игры с бонусом — активируйте промокод и начните выигрывать уже сегодня!