JUST RELEASED - TRANSPLANTATION - NOVEMBER ISSUE
This month gives you a round-up of the issues that the pandemic has inflicted on transplantation globally – both clinical issues and program management come under scrutiny across the world. In some senses these papers are emphasizing that everyone is dealing with the same clinical problems in transplant recipients and in other ways the differences show us the impact of the environment on the work we do. Research work across the field of transplantation has been impacted but there is much in this issue to contemplate as we plan the next phase of transplantation-under-COVID conditions.
CLICK HERE TO ACCESS THIS ISSUE
TTS MEMBERS - CLICK HERE TO SIGN-IN FOR OPEN ACCESS THROUGH TTS.ORG
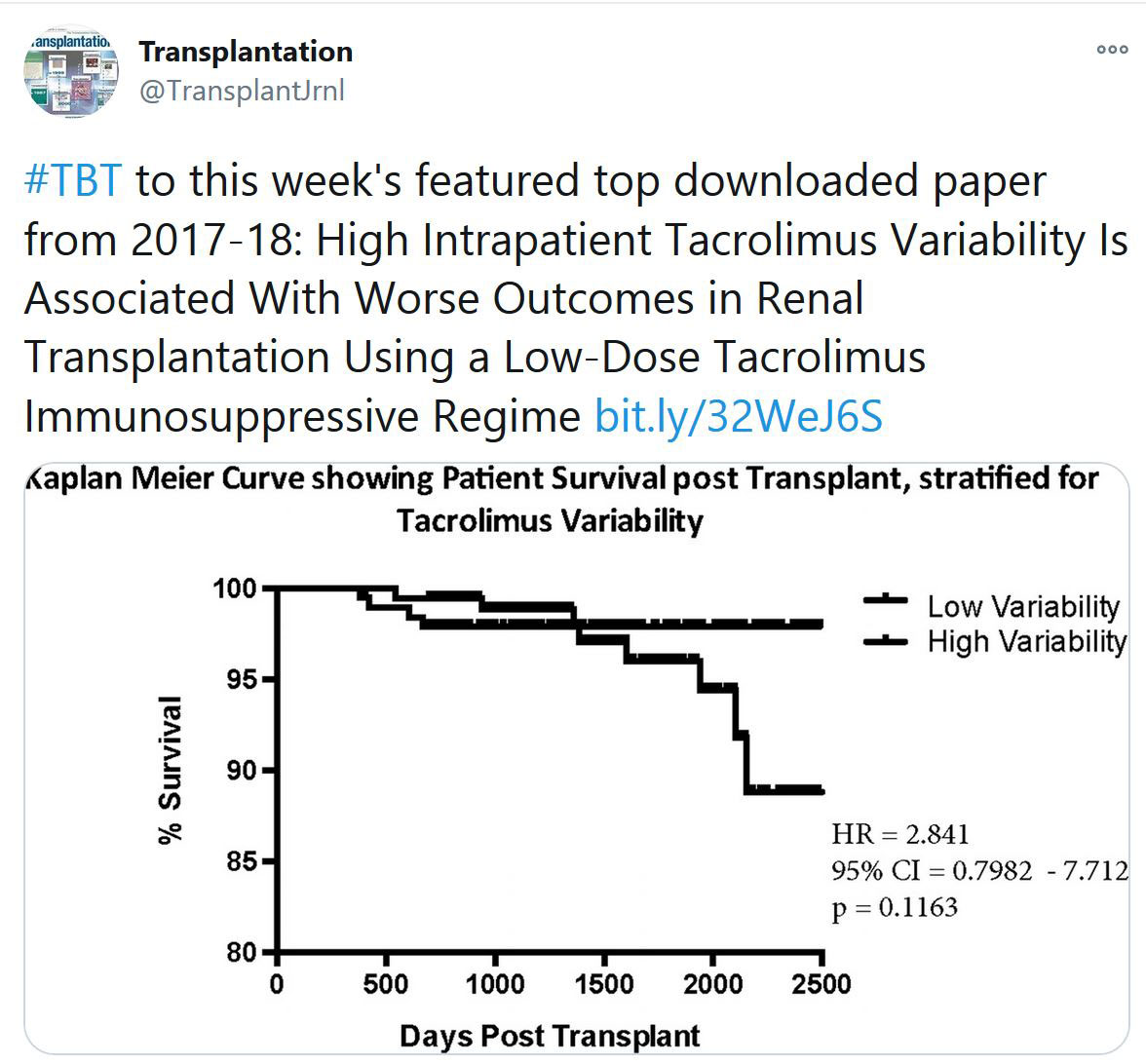
TRANSPLANTATION - WEEK'S MOST DOWNLOADED PAPER
JUST RELEASED - TRANSPLANTATION DIRECT - NOVEMBER ISSUE
The November issue of Transplantation Direct is out! It starts with a commentary (R. Bernstein Mannon) on an important review article in this issue regarding gender disparities in publications, citations and funding in the field of transplantation (Benjamens et al). We also have two letters discussing aspects of a recent Direct article on balancing costs/efficiency when screening donors for malignancies by whole body CT scan. Another interesting letter describes the effects of COVID-19 on liver transplantation in the Eurotransplant region. In kidney transplantation there is a study on donor-derived cell-free DNA as a predictor of BK virus-associated nephropathy. Articles in liver transplantation focus on analyses of etiologic trends and outcomes related to alcoholic hepatitis as a cause for organ replacement; an exploratory study is presented on using serial ultrasound of the rectus femoris muscle area on patients in the ICU as an indicator of mortality rate. In heart transplantation, mitochondrial-related gene activity is tested as a gauge for acute cardiac allograft rejection, and another study investigates exosome profiling (C4d) to detect antibody-mediated rejection. There are also articles on using hepatocyte growth factor to enhance the function of encapsulated xeno-pancreatic islets, and on studying factors in pancreas explants that affect islet stability for transplantation. On the topic of ethics, the complexities of DCD heart transplantation are examined and the authors have developed decision-making diagrams to help in these difficult clinical situations. There is plenty to discover in this issue of Transplantation Direct; please visit our website for the full open-access articles.
TRANSPLANTATION - HIGHLIGHTED ARTICLE
Dr. Jeremy R. Chapman, Editor-in-Chief, Transplantation
Biomarkers of Cytokine Release Syndrome Predict Disease Severity and Mortality From COVID-19 in Kidney Transplant Recipients
Benotmane I, Perrin P, Gautier Vargas G, et al.
Transplantation: September 30, 2020 - Volume Online First
We are all challenged by the management of sick patients resulting from the COVID-19 pandemic, not least in kidney transplant patients where the data are sparse. France has been amongst the hardest hit populations and this study of 49 patients adds to our knowledge of the risk factors for severity. A total of 49 patients were divided into 8 with mild disease, 21 hospitalised but not severely ill and 20 with severe disease. The 30-day mortality rate in hospitalized patients was 19.5%. Early elevations of C-reactive protein (>100 mg/L) and interleukin-6 (>65 ng/L) followed by increases in high-sensitivity troponin I (>30 ng/L) and D-dimer (>960 ng/mL) were significantly associated with severe disease and mortality. Viral load did not have prognostic significance. The study helps in determining optimal monitoring of our patients and may lead to improved outcomes.
Upcoming Webinars
IPTA ALLIED HEALTH AND NURSING PROFESSIONALS WEBINAR
TIPS AND TRICKS FOR VIRTUAL CARE IN PEDIATRIC TRANSPLANT
The COVID -19 pandemic has been a time of rapid and unprecedented change in the provision of clinical care. Both health care professionals and the transplant families we provide care for have had to adjust to this change at a monumental pace.
This session is meant to highlight some of the adaptations made by various members of our transplant allied health and nursing professional community whose practice has traditionally relied upon in-person assessment and intervention.
The session will have presentations from the following professionals from across the globe:
- Clinical Psychologists
- Physiotherapist
- Physician Assistant
- Child Life Specialist
Objectives:
- Develop a greater understanding of varying allied health and nursing clinical practice adaptations during the COVID-19 pandemic
- Review the learned pros and cons of virtual practice and adaptations made
- Discuss potential longer term practice changes that have evolved as a result of the pandemic
DATE/TIME CHANGE
ISN-TTS Webinar: Donor/Recipient pair - Risks vs. Gains - Cancer
«HOT OFF THE PRESS»
RECENT PUBLICATIONS IDENTIFIED BY TTS EDUCATION COMMITTEE ON COVID-19
Robust neutralizing antibodies to SARS-CoV-2 infection persist for months
Ania Wajnberg et al.
Science. 10.1126/science.abd7728 (2020)
This article reported that the vast majority of infected individuals with mild-to-moderate COVID-19 experience robust IgG antibody responses against the viral spike protein, based on a dataset of 30,082 individuals screened at Mount Sinai Health System in New York City. More than 90% of seroconverters make detectible neutralizing antibody responses. The titers are relatively stable for at least a period approximating 5 months and that anti-spike binding titers significantly correlate with neutralization of authentic SARS-CoV-2.
Compromised humoral functional evolution tracks with SARS-CoV-2
Tomer Zohar et al.
Cell. DOI: https://doi.org/10.1016/j.cell.2020.10.052
This article dissected the early evolution of the humoral response in 193 hospitalized individuals ranging from moderate-to severe. Although robust IgM and IgA responses evolved in both survivors and non-survivors with severe disease, non-survivors showed attenuated IgG responses, accompanied by compromised Fcɣ-receptor binding and Fceffector activity, pointing to deficient humoral development rather than disease-enhancing humoral immunity. In contrast, individuals with moderate disease exhibited delayed responses that ultimately matured. These data highlight distinct humoral trajectories associated with resolution of SARS.
Incidence, Characteristics, and Outcome of COVID-19 in Adults on Kidney Replacement Therapy: A Regionwide Registry Study
Johan De Meester et al.
JASN. doi: https://doi.org/10.1681/ASN.2020060875
This study conducted a prospective, multicenter, region-wide registry study in adult patients on RRT versus the general population from March 2 to May 25, 2020 in Belgium. At the end of the epidemic wave, crude and age-standardized cumulative incidence rates of SARS-CoV-2 infection were 5.3% versus 2.5%, respectively, among 4297 patients on hemodialysis, and 1.4% versus 1.6%, respectively, among 3293 patients with kidney transplants (compared with 0.6% in the general population). Crude and age-standardized cumulative mortality rates were 29.6% versus 19.9%, respectively, among patients on hemodialysis, and 14.0% versus 23.0%, respectively, among patients with transplants (compared with 15.3% in the general population). This found no excess mortality in the hemodialysis population when compared with mean mortality rates during the same 12-week period in 2015–2019 because COVID-19 mortality was balanced by lower than expected mortality among uninfected patients.
TTS and TTS Sections News
IPTA 2020 Call for Nominations
The IPTA Nominations Committee is seeking qualified candidates to be considered for open Councilor and Officer positions beginning in May 2021.
All applications will be reviewed by the IPTA Nominations Committee, who will present a final slate of candidate officers and councilors to the IPTA membership for the 2021 election.
The IPTA Nominations Committee welcomes nominations and applications from anyone who has been an IPTA member in good standing for at least 1 year. Service to IPTA on committees or special activities relevant to the society is an asset.
The deadline for online submission of applications is November 30, 2020.
TTS 2020

Young Member's Committee Chair, Shaifali Sandal interviewed Elmi Muller and Dorry Segev where she asked questions relevant to those new to the transplant community.
CORONAVIRUS (COVID-19) UPDATES
The Transplantation Society (TTS) and our journal Transplantation have developed online resources to keep you informed on the Coronavirus (COVID-19) outbreak.
- TTS Coronavirus (COVID-19) Dashboard
www.tts.org/covid-19 - Transplantation Global Transplantation COVID Report
www.tts.org/txjcovid19
We are also requesting contributions and news from the transplant community to be sent to covid-19@tts.org for inclusion on our resources page.
In this dashboard, you will find links to TTS and other global and regional resources, as well as interactive maps, publications and webinars. We encourage you to explore this dashboard and share with your colleagues.
Editors and contributors to Transplantation have shared their thoughts on how they are dealing with the current crisis. While we understand that the information of today may be quite different tomorrow in this fast-moving pandemic, this report will open our forum of an international exchange on COVID for the transplant community.
Website - www.tts.org/txjcovid19
Please send your own contributions and news to covid-19@tts.org for inclusion on our resources page.
IN THE NEWS
Changes in U.S. Allocation Policies for Donated Livers and Lungs
Nov. 4 - In the past, donated livers and lungs were generally offered first to the sickest patients within a donation service area (a location with fixed boundaries). But U.S. policies have changed. Now, these organs are typically offered first to the sickest patients who are a specified distance from the donor hospital—allowing sick patients to be eligible for organs that are donated across larger geographic areas.
Important considerations for drugs, nutritional, and herbal supplements in pediatric solid organ transplant recipients
Nov. 5 - Pediatric transplant recipients are on multiple prescription and non-prescription drugs. Many patients also use dietary, nutritional, and herbal supplements. This manuscript researched formulations of immunosuppressive drugs currently available and presents information on generic immunosuppressive drugs, commonly used non-prescription medications, dietary supplements, and herbal supplements. Immunosuppressive drugs are available in various formulations.
Notable Variation Exists in the Treatment of Serious VTE Events in Pediatric Leukemia
Nov. 5 - Among hematology, oncology, and bone marrow transplant practitioners, notable variations in practice regarding the treatment of serious venous thromboembolism (VTE) events, pulmonary embolism (PE), and cerebral venous sinus thrombosis (CVST), were noted in children with leukemia, according to survey results.
Racial Disparities in Kidney Transplantation Start Downstream of Referral
Nov. 6 - Investigators have identified when during the transplant evaluation process racial disparities occur. Results of the new study comparing 23,499 Black and 36,730 White patients starting dialysis were presented during the American Society of Nephrology’s Kidney Week 2020 Reimagined virtual conference.
UPCOMING MEETINGS AND ANNOUNCEMENTS
International Transplantation Science Meeting (ITS 2021)

IPITA-IXA-CTRMS Joint Congress
Asian Transplantation Week (ATW) 2020
Contact
Address
The Transplantation Society
International Headquarters
740 Notre-Dame Ouest
Suite 1245
Montréal, QC, H3C 3X6
Canada
Используйте Вавада казино для игры с бонусом — активируйте промокод и начните выигрывать уже сегодня!